Precision training
Training relies heavily on the feedback of the therapists, again based on observation and experience.

Innovation is more than a buzzword for us. Equipped with our own clinical research team and thanks to our strong research collaborations, we do not only implement innovative technologies into our practices as fast as possible, but we also test their efficiency in treatment.
The goal of our research partnerships is to develop a novel form of neurorehabilitation that is seamlessly integrated into the daily routine of our patients. The goal is that you train yourself by being as active as possible. The necessary corrective feedback, assistance and safety measures are provided by intelligent technology and by the interaction with your therapist.
We are continuously taking part in innovative research collaborations and projects working in conjunction with renowned educational bodies around the world and always aiming for the highest quality in neurorehabilitation, based on the latest scientific developments.
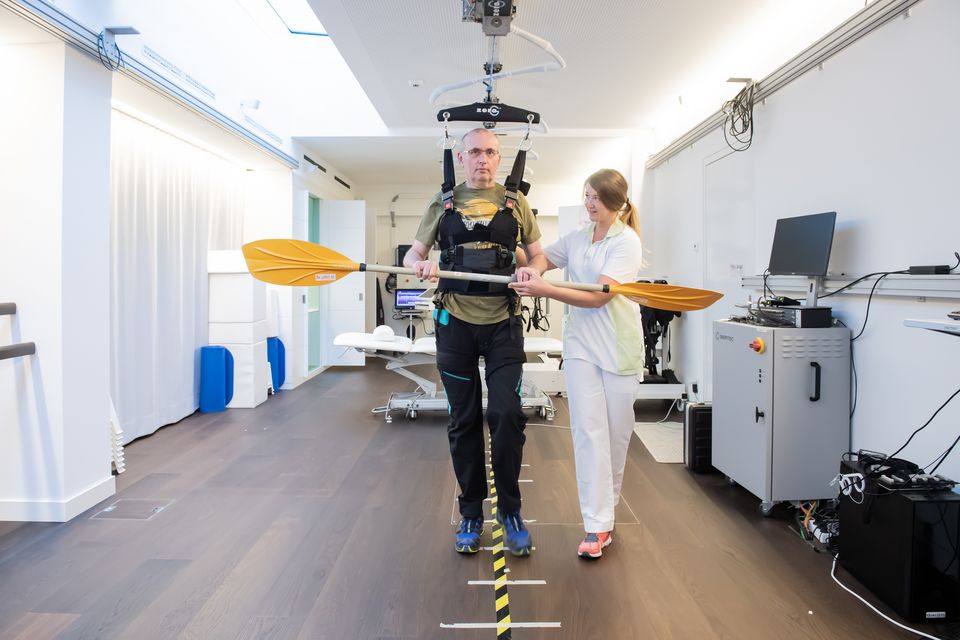
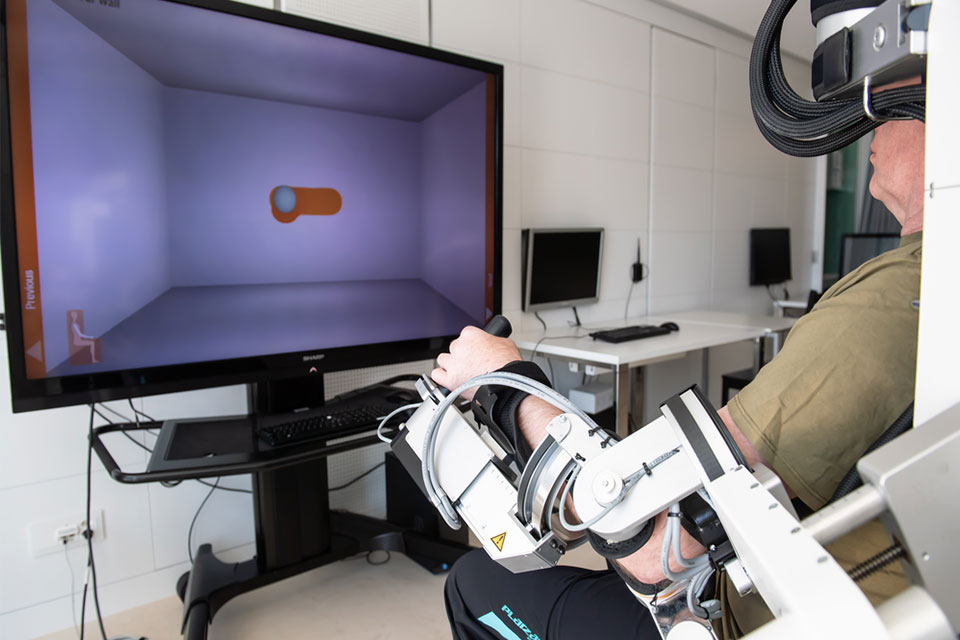







Our neurorehabilitation clinics are equipped with state-of-the-art movement analysis, robotic systems and other innovative devices to complement the hands-on training with the therapist.
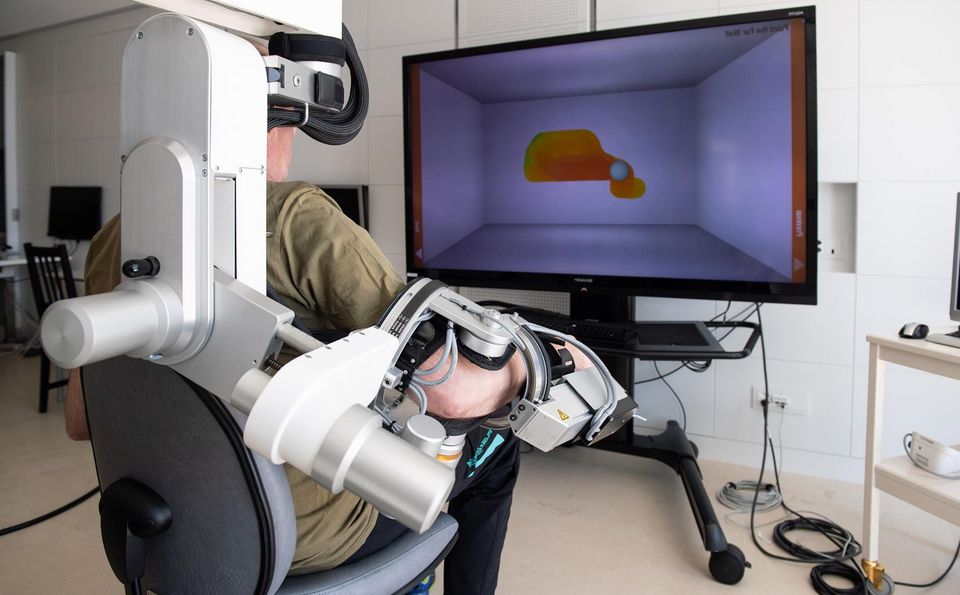
Armeo® Power by Hocoma
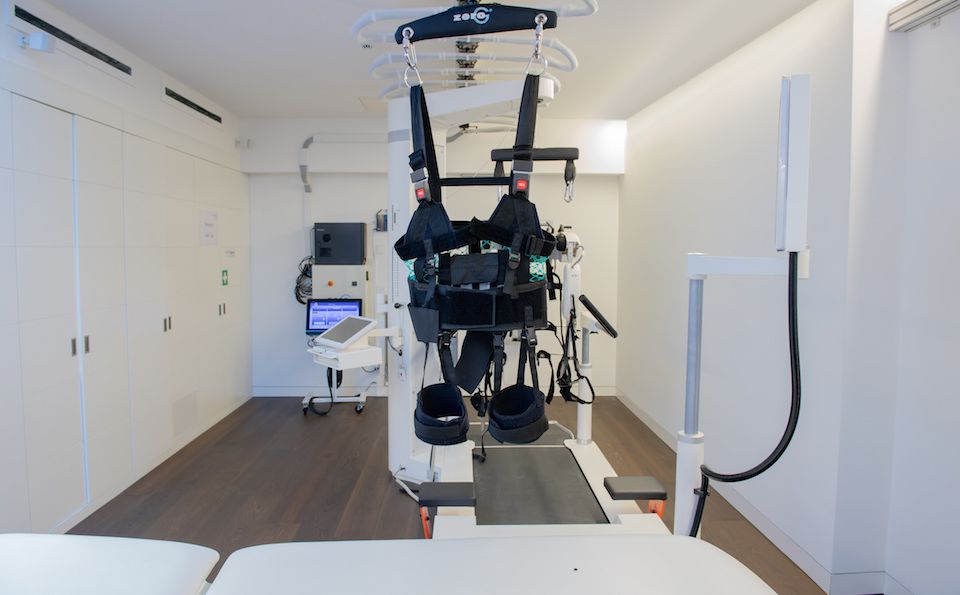
ZeroG® by Aretech

Split-belt treadmill
Together with the cereneo Institute for Interdisciplinary Research (cefir), the University Hospital of Zurich and the ETH (Technical University), we perform basic and clinical research including randomised controlled trials testing new training and diagnostic methods.
Training relies heavily on the feedback of the therapists, again based on observation and experience.
The continuous evaluation of neurological impairments and disability are the backbone of targeted and successful rehabilitation therapy
Based on evidence that we developed in our basic science program, we hypothesise that training can be improved by adding rewards.
Dr Meret Branscheidt, Medical Director at the cereneo Rehabilitation Center Hertenstein has been part of the NIBS roundtable expert team to establish a translational roadmap for the use of precision non-invasive brain stimulation in stroke rehabilitation. The outcome of this expert roundtable is the establishment of 5 key recommendations for the use of NIBS with the goal to tailor NIBS to the specific patient needs by using the same set of measurements to better track results to compare different studies.
At cereneo, Dr Meret Branscheidt is successfully using the different NIBS techniques at the cereneo rehabilitation clinic in Switzerland to support the recovery of stroke patients.
This is a case report by Mike D. Rinderknecht, Julio A. Dueñas, Jeremia P. Held, Olivier Lambercy, Fabio M. Conti, Leopold Zizlsperger, Andreas R. Luft, Marie-ClaudeHepp-Reymond and RogerGassert. The report describes a novel automated assessment tool for tactile mislocalization in neurological patients with somatosensory deficits after stroke. The automated assessment tool allows to identify, locate, precisely quantify, and depict the patients’ deficits in topesthesia, which can be severely affected by neurological injuries, such as stroke.
This longitudinal study by Jing Xu, Meret Branscheidt, Heidi Schambra, Levke Steiner, Mario Widmer, Jörn Diederichsen, Jeff Goldsmith, Martin Lindquist, Tomoko Kitago, Andreas R. Luft, John W. Krakauer and Pablo A. Celnik aims to investigate inter hemispheric interactions of stroke patients by tracking their pre-movement inter hemispheric inhibition (IHI) for one year following their stroke. An inhibitory imbalance found in patients with chronic stroke seems to correlate with poor motor performance and is a target for therapeutic interventions.
This study by Heidi M. Schambra, Jing Xu, Meret Branscheidt, Martin Lindquist, Jasim Uddin, Levke Steiner, Benjamin Hertler, Nathan Kim, Jessica Berard, Michelle D. Harran, Juan C. Cortes, Tomoko Kitago, Andreas Luft, John W. Krakauer and Pablo A. Celnik aims to determine if presence or absence of motor evoked potentials (MEPs) differentially influences recovery of volitional contraction and strength in an arm muscle versus an intrinsic hand muscle. Recovery of movement in proximal and distal upper extremity (UE) muscles after stroke appears to follow different time courses which suggests differences in their neutral substrates.
This prospective cross-sectional observational study by Anne Schwarz, Miguel M. C. Bhagubai, Saskia H. G. Nies, Jeremia P. O. Held, Peter H. Veltink, Jaap H. Buurke and Andreas R. Luft aims to comprehensively characterize spatiotemporal kinematics of stroke subjects during upper limb daily living activities. Therefore, kinematic expressions were investigated with respect to different movement types and impairment levels for the entire task as well as for motion subphases.
A prospective observational cohort study in stroke subjects by Jeremia P. O. Held, Anne Schwarz, Johannes Pohl, Eva Thürlimann, Silvan Porrtmann, Meret Branscheidt, Madalina Fratian, Jannie van Duinen, Janne M. Veerbeek and Andreas R. Luft. This study investigates the impact of the COVID-19 shutdown on stroke survivors’ access to therapy, physical activity, functioning and mood in Switzerland.
A prospective, longitudinal, observational cohort study by Bea Essers, Annick Van Gils, Christophe Lafosse, Marc Michielsen, Hilde Beyens, Fabienne Schillebeeckx, Janne M. Veerbeek, Andreas R. Luft, Daphne Kos and Geert Verheyden: The aim is to investigate the evolution of a group of stroke patients from six to 12 months, to determine factors on admission to inpatient rehabilitation. A shown ‘mismatch’ group of patients with good observed upper limb (UL) motor function but low perceived UL activity at six months post stroke tends to use the affected UL less in daily life than would be expected based on clinical tests. The importance of tailoring to the individual needs of patients is to be confirmed.
This study by Jeremia Philipp Oskar Held, Kevin Yu, Connor Pyles, Janne Marieke Verbeek, Felix Bork, Sandro-Michael Heining, Nassir Navab, Andreas R. Luft aims (1) to investigate manipulation of the gait pattern of persons who have had a stroke based on virtual augmentation during overground walking compared to walking without augmented reality (AR) performance feedback and (2) to investigate the usability of the AR system. Improving balance and gait are among the main goals of rehabilitation after stroke.
This study by Christoph M. Kanzler, Anne Schwarz, Jeremia P. O. Held, Andreas R. Luft, Roger Gassert and Olivier Lambercy evaluates the ability of the Virtual Peg Insertion Test (VPIT) to characterize arm and hand sensorimotor impairments that are relevant for performing functional tasks after stroke. To optimise the impact of neurorehabilitation interventions, it is essential to assess arm and hand sensorimotor impairments that are functionally relevant. The VPIT addresses limitations and quantifies movements during a goal-directed manipulation task.
This Delphi study by Johannes Pohl, Jeremia Philipp Oskar Held, Geert Verheyden, Margit Alt Murphy, Stefan Engelter, Agnes Flöel, Thierry Keller, Gert Kwakkel, Tobias Nef, Nick Ward, Andreas R. Luft, Janne Marieke Veerbeek aims to develop an internationally agreed on core set of motor outcome measures for clinical application to serve as a quality standard in clinical motor rehabilitation post stroke.
This study by Anne Schwarz, Miguel M. C. Bhagubai, Gerjan Wolterink, Jeremia P. O. Held, Andreas R. Luft and Peter H. Veltink aims to improve the understanding of the pathophysiology of upper limb movement deficits and to prove the effectiveness of interventions after strokes.
The study by D. Flury, F. Massé, A. Paraschiv‑Ionescu, K. Aminian, A. R. Luft and R. Gonzenbach shows that information about motor performance in daily life can be valuable for tailoring rehabilitative therapy plans and counseling according to the needs of individual stroke patients.
A randomized controlled trial by Mario Widmer, Jeremia P. O. Held, Frieder Wittmann, Belen Valladares, Olivier Lambercy, Christian Sturzenegger, Antonella Palla, Kai Lutz, Andreas R. Luft: Learning and learning-related neuroplasticity in motor cortex are potential mechanisms mediating recovery of movement abilities after stroke. These mechanisms depend on dopaminergic projections from midbrain that may encode reward information. Likewise, therapist experience confirms the role of feedback/reward for training efficacy after stroke.
Mario Widmer, Kai Lutz and Andreas R. Luft (2019). Reduced striatal activation in response to rewarding motor performance feedback after stroke. NeuroImage: Clinical, Volume 24, 102036.
Robinson Kundert, MSc1,2,3, Jeff Goldsmith, PhD4*, Janne M. Veerbeek, PhD1,2, John W. Krakauer, MD5*, and Andreas R. Luft, MD1,2 (2019). Neurorehabilitation and Repair 00 (0): 1-12.
Burgos R, Bretónb I, Cereda E, Desport JC, Dziewas R, Genton L, Gomes F, Jésus P, Leischker A, Muscaritoli M, Poulia KA, Preiser JC, Van der Marckm M, Wirth R, Singer P, Bischoff S. (2017). ESPEN Guideline Clinical Nutrition in Neurology. Clin Nutr. 37: 354-396
Zizlsperger L, Kümmel F, Haarmeier T (2016) Metacognitive Confidence Increases with, but Does Not Determine, Visual Perceptual Learning. PLoS ONE 11(3): e0151218. doi:10.1371/journal. pone.0151218
Widmer, M., Held, J. P., Wittmann, F., Lambercy, O., Lutz, K., & Luft, A. R. (2017). Does motivation matter in upper-limb rehabilitation after stroke? ArmeoSenso-Reward: study protocol for a randomized controlled trial. Trials, 18(1), 580
Widmer, M., Stulz, S., Luft, A. R., & Lutz, K. (2017). Elderly adults show higher ventral striatal activation in response to motor performance related rewards than young adults. Neuroscience letters, 661, 18-22
Rasmussen, P., Widmer, M., Hilty, M. P., Hug, M., Sørensen, H., Ogoh, S., … & Lundby, C. (2017). Thermodilution-determined Internal Jugular Venous Flow. Medicine and science in sports and exercise, 49(4), 661-668
Xu, J., Ejaz, N., Hertler, B., Branscheidt, M., Widmer, M., Faria, A. V., … & Kitago, T. (2017). Separable systems for recovery of finger strength and control after stroke. Journal of neurophysiology, 118(2), 1151-1163
M. Widmer, N. Ziegler, J. Held, A. Luft, K. Lutz (2014). The influence of feedback on motor skill learning. Progress in Brain Research, Volume 229, ISSN 0079-6123, http://dx.doi.org/10.1016/bs.pbr.2016.05.006
Wittmann et al. Journal of NeuroEngineering and Rehabilitation (2016) 13:75. DOI 10.1186/s12984-016-0182-1
Gomes F., Emery P. W., Weekes C.E. (2016). Risk of Malnutrition Is an Independent Predictor of Mortality, Length of Hospital Stay, and Hospitalization Costs in Stroke Patients. Journal of Stroke and Cerebrovascular Diseases. 25(4): 799-806
Bounoure L, Gomes F, Stanga Z, Keller U, Meier R, Ballmer P, Fehr R, Mueller B, Genton L, Norman K, et al. (2016). Detection and treatment of medical inpatients with or at-risk of malnutrition: suggested procedures based on validated guidelines. Nutrition. 32(7-8): 790-8
Frieder Wittmann, Olivier Lambercy, Roman R. Gonzenbach, Mark A. van Raai, Raphael Höver, Jeremia Held, Michelle L. Starkey, Armin Curt, Andreas Luft and Roger Gassert (2015). IEEE International Conference on Rehabilitation Robotics (ICORR)
Kai Lutz, Mario Widmer (2014). Neuroscience and Neuroeconomics 2014:3
Bart Klaassen1, Bert-Jan van Beijnum, Marcel Weusthof, Dennis Hofs, Fokke van Meulen, Henk Luinge, Alessandro Tognetti, Federico Lorussi, Rita Paradiso, Jeremia Held, Jasper Reenalda, Corien Nikamp, Jaap Buurke, Hermie Hermens and Peter Veltink (2014).
F. Gomes, C. Hookway & C. E. Weekes (2013). Journal of Human Nutrition and Dietetics- The British Dietetic Association Ltd
James Sulzer, Ranganatha Sitaram, Maria Laura Blefari, Spyros Kollias, Niels Birbaumer, Klaas Enno Stephan, Andreas Luft, Roger Gassert (2013). J. Sulzer et al. / NeuroImage 83 (2013) 817–825
Meier ML, Bru¨gger M, Ettlin DA, Luechinger R, Barlow A, Jäncke L, Lutz K. Brain activation induced by dentine hypersensitivity pain–a fMRI study. J Clin Periodontol 2012; 39: 441–447. doi: 10.1111/j.1600-051X.2012.01863.x.
Afshin A. Divani, Shahram Majidi, Anna M. Barrett, Siamak Noorbaloochi and Andreas R. Luft (2011). American Heart Association, Inc. Stroke is available at http://stroke.ahajournals.org DOI: 10.1161/STROKEAHA.110.607630
Jonas A. Hosp, and Andreas R. Luft (2011). Neural Plasticity Volume 2011, Article ID 871296, 9 pages doi:10.1155/2011/871296
Jonas A. Hosp, Ana Pekanovic,Mengia S. Rioult-Pedotti, and Andreas R. Luft (2011). The Journal of Neuroscience, February 16, 2011 • 31(7):2481–2487 • 2481
Zina-MaryManjaly, Andreas R. Luft, and Hakan Sarikaya (2011). Case Reports in Neurological Medicine Volume 2011, Article ID 474271, 3 pages doi:10.1155/2011/474271